Oxidative Stress: The Hormone Connection
News & Science Behind Formulas • Related Resources & Links • Monthly Discount & Other Offers
Does Diagnosis Really Matter?
Oxidative Stress is a term that continues to garner greater attention and awareness among the general public and within mainstream medical practice. The term speaks to a basic premise of imbalance within the body, though the molecular mechanisms that drive this process are far from basic. One may consider why a fundamental understanding of oxidative stress is even relevant for those outside of the biological research or medical professions. After all, health and longevity are ultimately dependent upon the presence or absence of disease, and thus the focus should remain on eliminating disease to restore health, right? Well, depending on who you ask, this understanding of health as a dichotomy (disease presence vs. disease absence) is technically correct, though grossly incomplete and misrepresented in mainstream culture.
One should first consider that disease (based on Western medicine) is nothing more than a descriptive name assigned to a cluster of symptoms and/or diagnostics used in part to standardize treatments in an overburdened healthcare system. In this regard, those diagnosed with a known disease could be viewed as “unhealthy”, whereas those who are “healthy” lack known disease. For example, consider the individual with chronic fatigue, frequent episodes of pain in the joints and tissues, and persistent lack of mental clarity, and yet, is classified as “healthy” for lack of diagnosis. The fact that diagnosis is lacking does not by default place one in the company of good health. Rather, patients and practitioners should begin to gauge health on a continuum as opposed to discrete categories, focusing greater attention on the underlying factors that drive disease processes, like oxidative stress.
Oxygen, Electrons, and Antioxidants
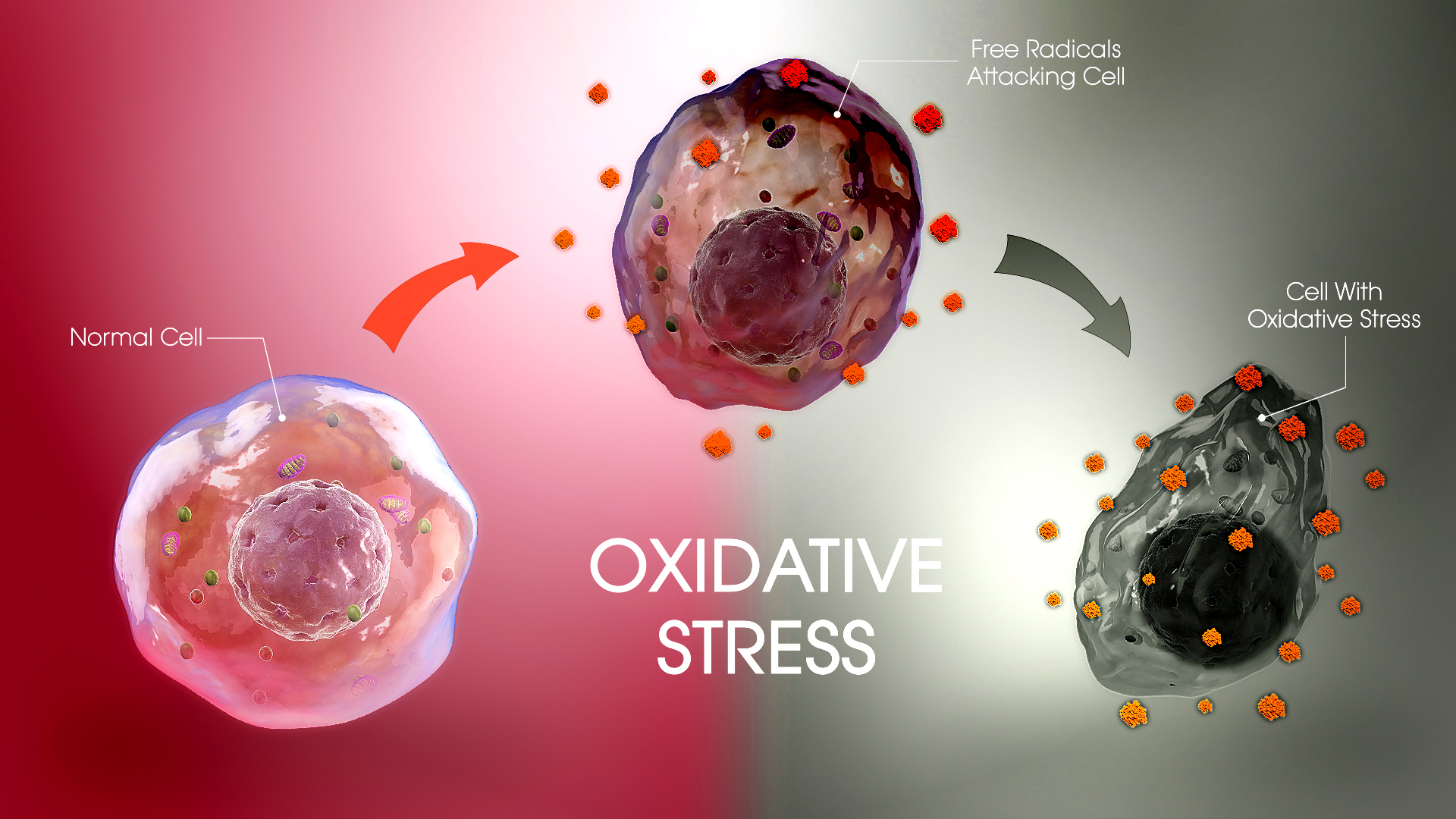
Oxidation is fundamental to the discussion of oxidative stress and degenerative diseases like Alzheimer’s, autoimmunity, heart disease, multiple sclerosis, osteoarthritis, cancer, and many other prevalent pathologies. Oxidation is essentially the loss of electrons from biological matter (e.g. cell lipids, proteins, organelles, etc.) through the addition of oxygen or removal hydrogen, whereas reduction is the gain of electrons through the addition of hydrogen or removal of oxygen. These processes form the basis of oxidative stress, which occurs when the homeostatic (healthy) balance between oxidative and reducing substances is disrupted in a way that contributes to cellular damage and creates inflammation – a function of the immune system that serves to protect and heal, while also creating disease and dysfunction when left uncontrolled.
It is important to understand that oxidative reactions are a fundamental consequence of aerobic life (Ursini et al., 2016), which is necessary to sustain the high energy demands of the body’s cells. However, the aerobic process of breathing oxygen also leads to production of reactive oxygen species (ROS) that can and do contribute to oxidative stress. Fortunately, the body is of capable of counterbalancing these oxidative challenges through an intricate system of internally and externally derived antioxidants.
For example, one of the major internally generated antioxidants in the body is reduced glutathione (GSH), while vitamins C and E offer externally-derived sources (Ma, 2013). These substances participate in the tightly regulated oxidative-reductive balancing needed to maintain normal physiological processes through the donation of electrons to stabilize cellular structures and molecules that would otherwise become damaged and dysfunctional. Problems in this oxidant-antioxidant balance begin to occur as a result of increased exposure to different reactive species with greater propensity to steal electrons at a rate exceeding the protective capacity of internal and external antioxidant defenses. Harmful reactive species stem from numerous and diverse sources, though toxicants (xenobiotics) in the environment, a diet high in refined/inflammatory foods, and psychological stress are primary considerations (Ursini et al., 2016).
Oxidative Stress and Hormones
It is helpful to understand what is meant by the terms “upstream” and “downstream” medicine. When it comes to medical diagnoses, downstream medicine is on display. Downstream medicine involves readily observable outcomes, such as a pattern of symptoms or laboratory markers that signify a distinct level of dysfunction or disease (e.g., Cancer, Type-2 Diabetes, Hashimoto’s Thyroiditis, etc.). Hormone imbalances, whether excessive or deficient, are very much within the spectrum of downstream medicine. This is because hormone production and/or availability in the body is the end-result of “upstream” processes that occur at a cellular level and involve the organelles of each cell, especially the mitochondria or endoplasmic reticulum, that must function correctly for hormones to be produced in first place. Unlike downstream medicine, upstream medicine tends to lack official diagnoses, but this does not make the dysfunction in a cell any less real. Upstream dysfunction in a cell tends to be present long before (often years) the downstream diagnosis is recognized. A good example of this involves autoimmunity. Autoantibodies may be present within a patient for many years, attacking and slowly destroying self-tissue, like the thyroid gland, yet the presence of disease is not recognized until thyroid hormones fall below an acceptable level of function, along with more noticeable symptoms that would prompt an individual to seek medical attention.
Hormone imbalances and dysfunction, in isolation or part of an official diagnosis, are quite often the product of oxidative stress. This understanding is well-established in medical research; however, the current approach to hormone imbalances typically involve a downstream approach, like insulin therapy in type-2 diabetes or testosterone replacement in hypogonadism for example. Hormone therapy can be very effective in reducing troubling symptoms or keeping labs within an acceptable range, yet this does not address the root of the problem which resides upstream. Hormone imbalances can result from a variety of influences, and there certainly is not a one-size-fits-all approach to improving imbalances in different endocrine cells and organs.
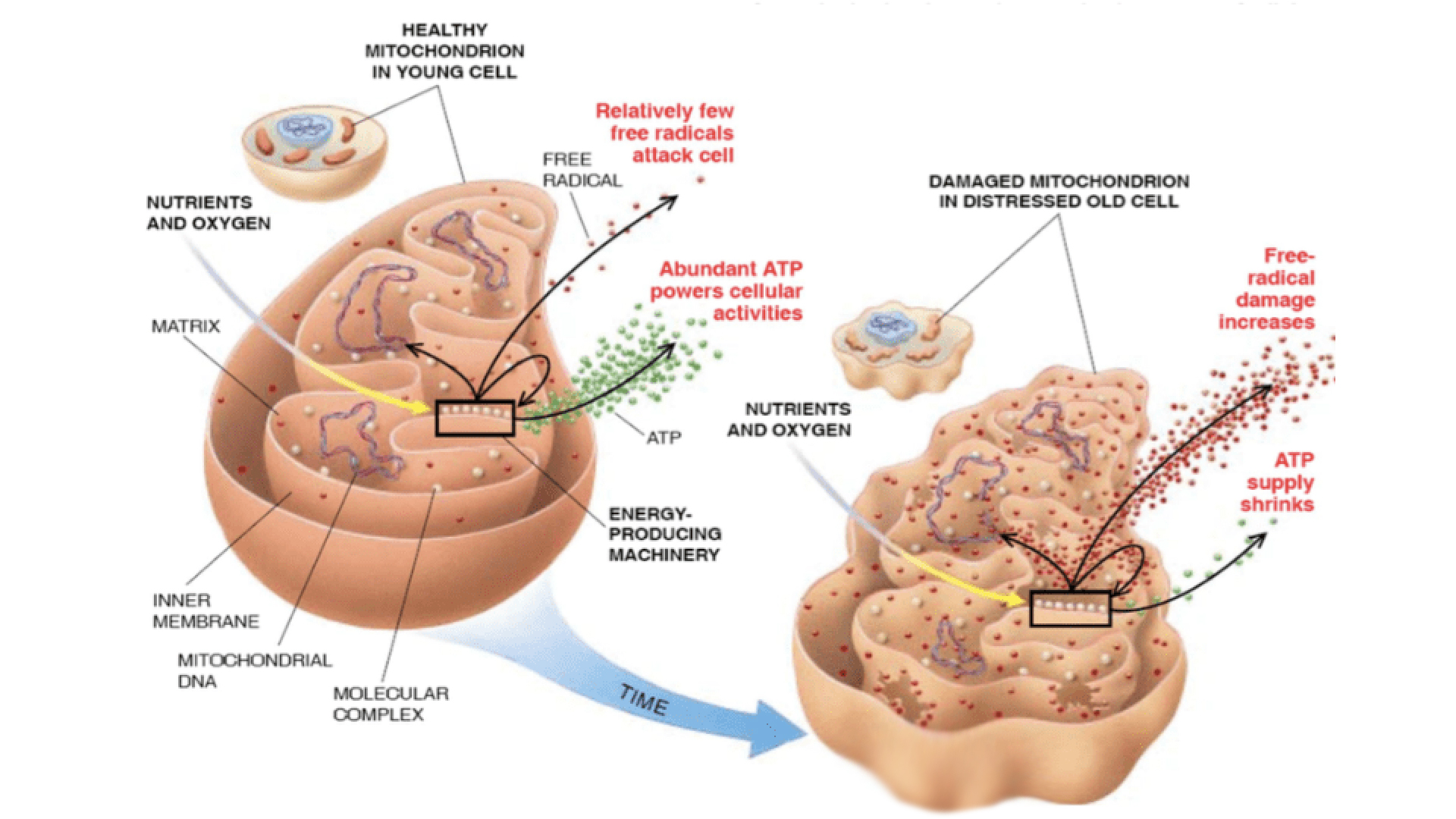
That said, a major target of upstream medicine in hormone imbalances involves the amelioration of oxidative stress within the cells, especially the mitochondria which are largely involved in the synthesis and utilization of hormones (Sergi et al., 2019; Lejri et al., 2018). Improving mitochondria health and function by correcting oxidative imbalances remains a key consideration for supporting healthy hormone levels at every age.
It is All About Balance
It is hoped that the relationship between oxidative stress, hormone imbalances, and disease is beginning to make a bit more sense at this point. Though the information presented herein offers a fundamental overview, there are multiple factors involved in the production of oxidative stress, as well as multiple strategies involving antioxidant and anti-inflammatory compounds that may be utilized to maintain a healthy oxidative-reductive balance, and thus support the healthy function of hormone-producing cells.
In closing, consider that health is not dependent on the diagnosis of disease. This is merely a label to facilitate symptom classification and treatment. Health should be viewed along a continuum, whereby oxidative-reductive status is maintained through avoidance of excessive oxidative and inflammatory exposures and balanced with the utilization of antioxidants that control oxidative stress and inflammation. As such, addressing the oxidative imbalances in the body remains a primary consideration in the prevention and treatment of most conditions, as opposed to simply eliminating symptoms that constitute a diagnosis.
References
1. Ma, Q. (2013). Role of nrf2 in oxidative stress and toxicity. Annual review of pharmacology and toxicology, 53, 401-26.
2. Lejri, I., Grimm, A., & Eckert, A. (2018). Mitochondria, Estrogen and Female Brain Aging. Frontiers in aging neuroscience, 10, 124.
3. Sergi, D., Naumovski, N., Heilbronn, L. K., Abeywardena, M., O’Callaghan, N., Lionetti, L., & Luscombe-Marsh, N. (2019). Mitochondrial (Dys)function and Insulin Resistance: From Pathophysiological Molecular Mechanisms to the Impact of Diet. Frontiers in Physiology.
4. Ursini, F., Maiorino, M., & Forman, H. J. (2016). Redox homeostasis: The Golden Mean of healthy living. Redox Biology, 8, 205-215.
Related Resources
• Men’s Health: Hormones & Aging ARTICLE – by Dr. Melissa Mitchell
• Gonadal Steroidogenic Pathways INFOGRAPHIC – printable pdf (free engagement tool)
Related Products & Ongoing Offers
— JULY 2020 OFFER —
Specific Nutraceutical Support for Hormones & Aging
- Andro-XY Plus (men)
- ProstaSpec (men)
- Bio-Zinc/C Chewable
- Bio-Zinc 50
- Adapt-Adren
- Bio-DHEA 25
- Mag Glycinate 510
- Mito-Detox III (60 caps, 120 caps)
- Bio D/K Plus
____________
Discount offer now expired
Other offers and discount may apply
— ONGOING PATIENT OFFER —
Free Shipping
Get FREE shipping on ALL orders
when you shop online at our public store.
No minimums. No code needed.
— PRACTITIONER OFFERS —

Free Brochures, Samples & More
- FREE educational brochures (bundled), shipped free of charge
- FREE product samples, including CBD
- FREE practitioner and patient price lists available by request
Contact us to fulfill your request.
B2B benefits for qualified professionals only.
Some restrictions may apply.
Medical Disclaimer: This content is for informational and educational purposes only. It is not intended to provide medical advice or take the place of such advice or treatment from a personal physician. All readers/viewers of this content are advised to consult their doctor or qualified health professional regarding specific health questions. Neither BioSpec Nutritionals, Practitioner Supply nor the publisher of this content takes responsibility for possible health consequences of anyone reading or following the information in this educational content. All viewers of this content, especially those taking prescription or over-the-counter medications, should consult their physicians before beginning any nutrition, supplement or lifestyle program.